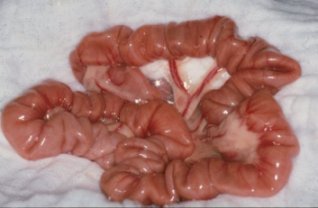
Estimada Dra. Patricia Permetei y amigos del Foro: Les mando este excelente artículo que encontre en la página del American Colege of veterinary Surgeron, en relacion a la presencia de cuerpos extranos en perros y gatos, con mucho afecto Dr. Jesús Villalobos; México.........Les mando una foto macroscopica de un intestino con apariencia de "acordeon" plegamiento por la presencia de un CE linealGASTROINTESTINAL FOREIGN BODIES Overview
Foreign bodies occur when animals consume items that will not readily pass through their gastrointestinal tract. These items can be a pet's or child's toy (Figures 1, 2 and 3) , strings (Figures 5 and 6) , leashes, clothing, sticks or any other item that fails to pass, including human food products like bones or trash. The problems that are caused vary with the duration that the foreign body has been present, the location of the foreign body, the degree of obstruction that is caused, as well as problems associated with the material of the foreign body. Some ingested items, like older pennies or lead material, can cause systemic toxicities while others may cause regional damage to the intestinal tract itself due to compression or obstruction. Gastrointestinal foreign bodies, especially strings, can often lead to perforation of the intestinal tract and spillage of intestinal contents into the abdomen. This condition quickly leads to inflammation of the abdominal lining (peritonitis) and allows bacterial proliferation and contamination (sepsis) which are both life threatening complications. While some small foreign bodies will pass, the majority will become lodged along the gastrointestinal tract and cause discomfort and clinical signs that may include inappetence, vomiting, diarrhea, lethargy, or abdominal pain. Some foreign bodies located in the stomach may be retrieved with the use of an endoscope; however, most require surgical abdominal exploration and removal. Occasionally, foreign bodies will become lodged in the esophagus at the base of the heart or at the diaphragm, which requires thoracic (chest) surgery. Causes
Nearly all gastrointestinal foreign bodies are items consumed by the pet. One exception is the rare trichobezoar (hairball). Incidence and Prevalence
Gastrointestinal foreign bodies are among the most common surgical emergencies in veterinary medicine. Younger animals are overwhelmingly predisposed to this condition. Cats are often diagnosed with linear foreign bodies due to ingestion of string or thread (with or without the needle). In contrast, dogs that frequently chew on objects usually are diagnosed with nonlinear foreign bodies. Signs and Symptoms
Clinical signs can vary significantly with the degree of obstruction, location, duration, and type of foreign body; however, vomiting, anorexia (loss of appetite), and abdominal pain are commonly noted. Other signs may include dehydration, diarrhea (with or without presence of blood), and in cases of linear foreign bodies, a string may be present wrapped around the base of the tongue or out of the anus. When to Seek Veterinary Advice
Vomiting, anorexia, diarrhea, and abdominal pain are all good reasons for evaluation by a veterinarian. The determination for referral to a surgical specialist is made by the primary veterinarian depending on diagnostics performed, the severity of the disease, and the facilities. Exam, Screening Tests, and Imaging
Most veterinarians require initial bloodwork that includes a complete blood count (CBC), serum chemistry, and a urinalysis. These combined will help to rule out other causes for vomiting, diarrhea, inappetence, anorexia, and abdominal pain. Abdominal, and occasionally thoracic, radiographs are regularly performed. Positive contrast radiographs (using barium to highlight the inside of the stomach and intestines) are regularly performed when routine radiographs fail to show the cause for the clinical signs. Ultrasound is also regularly performed. Additional tests that may be recommended include bloodwork to rule out specific metabolic diseases, fecal analysis to rule out parasites, as well as others that may be recommended by the veterinarian attending to your pet. Differential Diagnosis
Many endocrine diseases, including hyperthyroidism, hypoadrenocorticism (Addison's disease), and others may initially appear similar to gastrointestinal foreign bodies; however, these usually occur in older pets. Neoplasia (cancer), especially intestinal masses, may appear with similar clinical signs, as do primary intestinal diseases like inflammatory bowel disease, pancreatitis, gastritis, and ulcers. Complications Caused by the Disease
Intestinal obstruction and protracted vomiting and diarrhea can cause significant metabolic changes within the body. Additionally, if the foreign body has perforated the intestinal wall and entered the thoracic or abdominal cavities, profound complications may follow. These may include peritonitis, sepsis, and death. Many foreign bodies are made of materials that are potentially toxic when absorbed. Lead and zinc are good examples that when consumed may lead to profound systemic disease if enough is absorbed. Treatment Options
Surgical intervention is not always required with gastrointestinal foreign bodies. Occasionally, the item ingested is small and smooth enough to pass through the gastrointestinal tract without causing damage or becoming lodged. Additionally, few foreign bodies may become lodged in the upper gastrointestinal tract (mouth, esophagus, and stomach) and may be removed with the use of a flexible endoscope. Frequently, conservative management and endoscopy fail to provide relief and surgical exploratory is warranted. Esophageal foreign bodies require thoracic (chest) surgery to gain access for removal. Most gastrointestinal foreign bodies become lodged within the stomach or intestines and require a gastrotomy (opening the stomach- Figure 2 above) or enterotomy (opening the intestines). Once the item has been removed, the gastrointestinal tract is closed. (Figure 4) Many linear foreign bodies and completely obstructed intestines are damaged severely enough that multiple enterotomies or an intestinal resection and anastomosis (procedure to remove a segment of the intestines and reattach the remaining portion) will be required. The decision of the procedure of choice is determined by the surgeon when all the intestines and other abdominal organs may be evaluated. Potential Complications Following Treatment
The leakage of intestinal contents into the abdomen and subsequent sepsis and peritonitis is always a risk during intestinal surgery, although meticulous care and adequate flushing of the abdomen usually prevent these. General anesthesia can always carry the risk of mortality and infection and dehiscence (breakdown of sutured tissues) is always risked during surgery. Dehiscence can occur at the site of the enterotomy, gastrotomy, or resection and anastomosis site, or at the closure to the abdominal wall. Aftercare
Many patients have a degree of metabolic illness secondary to the obstruction caused by the foreign body and will need to be treated symptomatically to return them to normal. Additionally, patients will need to be monitored to ensure that they return to eating and that their clinical signs resolve. Finally, evaluation for presence of intestinal or stomach dehiscence will need to be done for 3-5 days postoperatively. Intravenous fluids and antibiotics are often given as needed. Prognosis
Most uncomplicated gastrointestinal foreign bodies carry an excellent prognosis. Most patients return to eating within 1-2 days and clinical signs resolve. The prognosis worsens if there is an increased duration of time until the patient is seen or the obstruction is detected. The location of the foreign body also may indicate a worse scenario. Linear foreign bodies can carry a good prognosis if they are resolved early in the course of the disease. As these become prolonged, the risk for perforation increases. Perforation and subsequent peritonitis and sepsis carry a guarded prognosis and will require additional operative and postoperative care. Greg Marsolais, DVM, MS
Small Animal Resident
Editor: William Daly, DVM
Diplomate ACVS Posted 8/13/2004 |